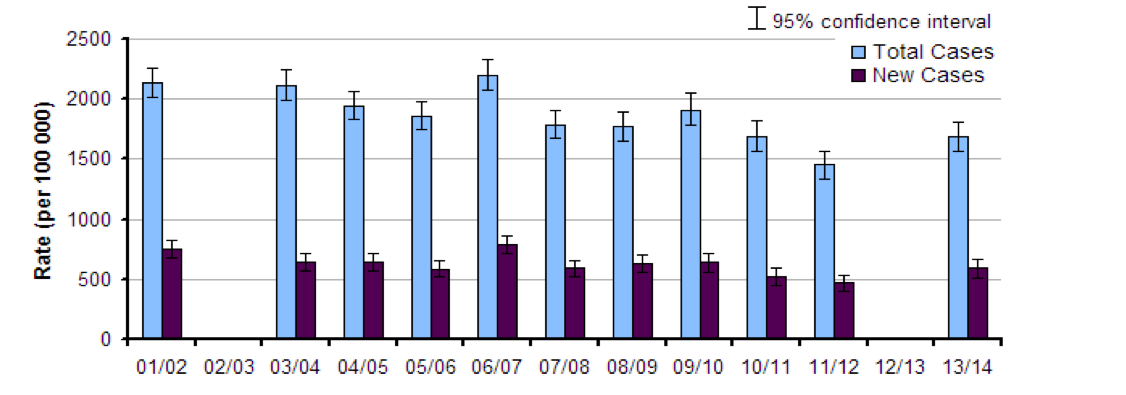
More than eight million working days were lost in the UK because of musculoskeletal disorders (MSDs) in 2013/14, according to the Labour force survey , published by the Office for National Statistics (ONS) in August 2014.
If you read nothing else, read this…
- Rapid diagnosis and treatment are ideal for tackling musculoskeletal disorders (MSDs).
- Education about health should encourage staff to make healthier choices.
- Exercise can be an effective tool to improve employee health and prevent or treat MSDs.
- Healthcare strategies should focus on the needs of the workforce while also considering costs.
The survey also found that MSDs caused by work-related activities accounted for 526,000 out of 1,241,000 working days lost through work-related illnesses in 2013/14. So what can employers do to support staff suffering from MSDs and thereby reduce absence levels?
Professor John Savill, chief executive of the Medical Research Council, says a better understanding is needed of how to maintain healthy working environments to minimise the impact of ill-health on productivity. This will become increasingly important as workforce demographics change as employees remain in work longer.
Early diagnosis and treatment of MSDs can help to minimise the length of absences. Mike Blake, compliance director at employee healthcare and risk management service provider PMI Health Group, says: “A reasonably swift diagnosis and treatment are ideal. The sooner something is done about it, the better.”
Another effective strategy is to identify possible causes of musculoskeletal issues in the workplace. Iain Loughran, physiotherapist and director at South Tyneside Foundation NHS Trust, says: “Some of the most effective strategies to support MSDs in the workplace are pre-employment assessments, workstation assessments, self-referral or early access to physiotherapy treatment, implementation of advice by managers, or reduced hours and job responsibilities for staff.”
Early intervention is more likely to result in an employee returning to work sooner, particularly if their employer operates a structured return-to-work programme, for example by operating a phased return to work or by making reasonable adjustments to an employee’s working environment.
Physiotherapy is a key tool to help staff overcome MSDs. Blake adds: “Ideally, employers need a selection of provisions in place to prevent musculoskeletal disorders. Larger employers could have an in-house physiotherapist, but that is not really financially suitable for smaller employers.”
Private medical insurance (PMI) and health cash plans can help staff to access and fund physiotherapy sessions.
Educating staff specifically about such issues, as well as giving them more general information about their health and wellbeing, can encourage them to make healthier lifestyle choices, which can help to prevent health problems.
For example, encouraging staff to exercise can help to guard against musculoskeletal issues and, in some cases, will reduce absences. Speaking at employee benefits network Maxis’ global conference in Paris in November 2014, professor Levon Doursounian, head of orthopaedic surgery at Hôpital Saint Antoine, says: “Workplace interventions should be used to promote physical activity because individuals with high support have higher levels of exercise.”
However, in England, 66% of men and 56% of women claim to meet the Chief Medical Officer’s recommendations in terms of the amount of physical activity they take part in, according to the Health and Social Care Information Centre’s 2013 Health survey for England: Is the adult population in England active enough? , published in July 2013.
Employers can facilitate physical activity by providing benefits such as on-site exercise classes, an on-site gym or corporate gym membership, for example, via a flexible or voluntary benefits scheme.
Who implements the strategies?
But, despite the obvious advantages for employers, some have questioned who should really be responsible for supporting staff suffering from MSDs, asking whether it should be down to employers to implement such initiatives, or should individuals or the NHS take more responsibility?
PMI’s Blake says: ”The individual, the NHS and employers are all responsible for health and wellbeing in the workplace. But the employer has the biggest load to bear and the most capacity for prevention.
“Line managers need a back-up plan to refer people into, which they can only do when there is a problem already, rather than as a preventative tool.”
Loughran adds: “Beyond cost, it is often down to what is practical, in that fit staff and those who are off sick are easy to manage. Staff on phased returns to work require more effort to accommodate.”
Budgeting and strategy
Supporting staff with MSDs can also reduce employers’ costs, even when the benefits spend is taken into account.
Mark Sharpe, rehabilitation clinical lead at healthcare provider Aviva UK Health, says musculoskeletal disorders are one of the largest contributors to workplace costs, so employers need to have a robust strategy in place to treat them.
Ensuring their healthcare budget is targeted to support employees’ needs will also improve employers’ return on investment.
In future, employers will be able to draw on the findings of a new research centre, the Arthritis Research UK/MRC Centre for Musculoskeletal Health and Work, led by the University of Southampton, which was announced in 2014, to inform their strategies.
Among other projects, the centre will research how the three main musculoskeletal causes of work disability, back, neck and arm pain, osteoarthritis and inflammatory arthritis, affect older staff who are approaching retirement age.
So, although preventing and treating MSDs can be challenging for employers, effective strategies tailored to the needs of their workforce, early intervention, swift diagnosis and a return-to-work strategy will prepare them well to support the health of their workforce.
Case study: Staffordshire county council reduces musculoskeletal-related absence

Staffordshire county council has reduced its level of musculoskeletal-related employee absence and absenteeism after introducing a suite of health initiatives in December 2013.
Before the initiatives, musculoskeletal disorders (MSDs) accounted for 30% of sick days for council staff. Although the organisation has not yet formally calculated how much this figure has fallen, anecdotally it has seen fewer musculoskeletal-related absences.
The council’s latest Achieving excellence quarterly performance report, published in March 2014, says that since December 2013, the average number of days lost through sickness overall has fallen to 7.06 days per employee per year from the previously figure of 7.2 days per employee. This is significantly below the national average of 8.6 days in the public sector and 7.7 in the private sector.
Ian Parry, deputy leader of Staffordshire county council , says staff are provided with physiotherapy and a counselling and therapy service that offers rapid assessment and treatment free of charge.
Managers can refer employees within 24 hours of them calling in sick, so that physiotherapists can assess their condition and begin treatment within 48 hours.
Parry says: “Ensuring that we support employees by identifying the main causes of absenteeism in the workplace is imperative. There are rewards to be gained from investing in workplace health for staff and employers.”
Estimated rates for total cases and new cases of work-related musculoskeletal disorders in Great Britain, for people working in the last 12 months (Source: LFS, August 2014)